Theo Von’s Sobering Antidepressant Story Is Only the Tip of a Much Bigger Problem
From emotional numbness to severe withdrawal, the real-world data tells a very different story than what patients are promised.
The following information is based on a report originally published by A Midwestern Doctor. Key details have been streamlined and editorialized for clarity and impact. Read the original report here.
Theo Von got personal on Joe Rogan’s podcast after revealing a sad story about his long-term struggle with antidepressants.
He told Rogan he was first put on antidepressants after “a tough day at school” and has NEVER been able to get off them since.
THEO: “That shit makes you feel dead, man.”
ROGAN: “So why did you take them in the first place?”
THEO: “Cause I was in a bad relationship 20 years ago, and I was having a tough day at school, and they f*cking gave them to me, and then I never got off.”
Theo’s experience is not uncommon.
A 2019 meta-analysis revealed that 56% of people experience withdrawal symptoms when trying to quit antidepressants.
Of those who experienced withdrawal symptoms, nearly half (46%) described them as “severe.”
Before you get placed on the antidepressant hamster wheel like Theo Von did, you should learn what these drugs really do.
The nasty withdrawal symptoms are just the tip of the iceberg of a much bigger problem.
Most people still believe antidepressants fix a “chemical imbalance” in the brain.
It’s one of the most successful ideas ever sold in medicine. Simple, intuitive, and repeated so often that it feels like established fact.
Hardly anyone questions it. Why would they?
But when you actually go looking for the evidence behind that claim, it becomes surprisingly hard to find anything solid supporting it.
SSRIs didn’t just become common—they became… everywhere.
They’re prescribed for a laundry list of challenges. Depression, anxiety, stress, burnout, grief—even the normal emotional ups and downs that come with life.
And because they’re so normalized, most people never stop to ask basic questions.
How well do they actually work? Are they even necessary?
According to the data, only a minority of patients truly benefit from SSRIs.
That doesn’t mean they never help anyone—but it does mean millions of people are taking a drug that may not be doing what they think it is.
And that’s where the disconnect begins.
This information comes from the work of medical researcher A Midwestern Doctor. For all the sources and details, read the full report below.
The Truth About SSRI Antidepressants
If a medication is being prescribed on a massive scale, but only works for a relatively small percentage of people, you would expect that to be a major point of discussion.
But it’s barely mentioned.
The assumption is still that if you’re struggling, this medication is the logical next step.
When Prozac first entered the market, the FDA received over 39,000 complaints in just the first nine years.
That’s not a handful of outliers.
That’s tens of thousands of signals, early on, that something wasn’t right.
And that’s a signal you’re supposed to listen to.
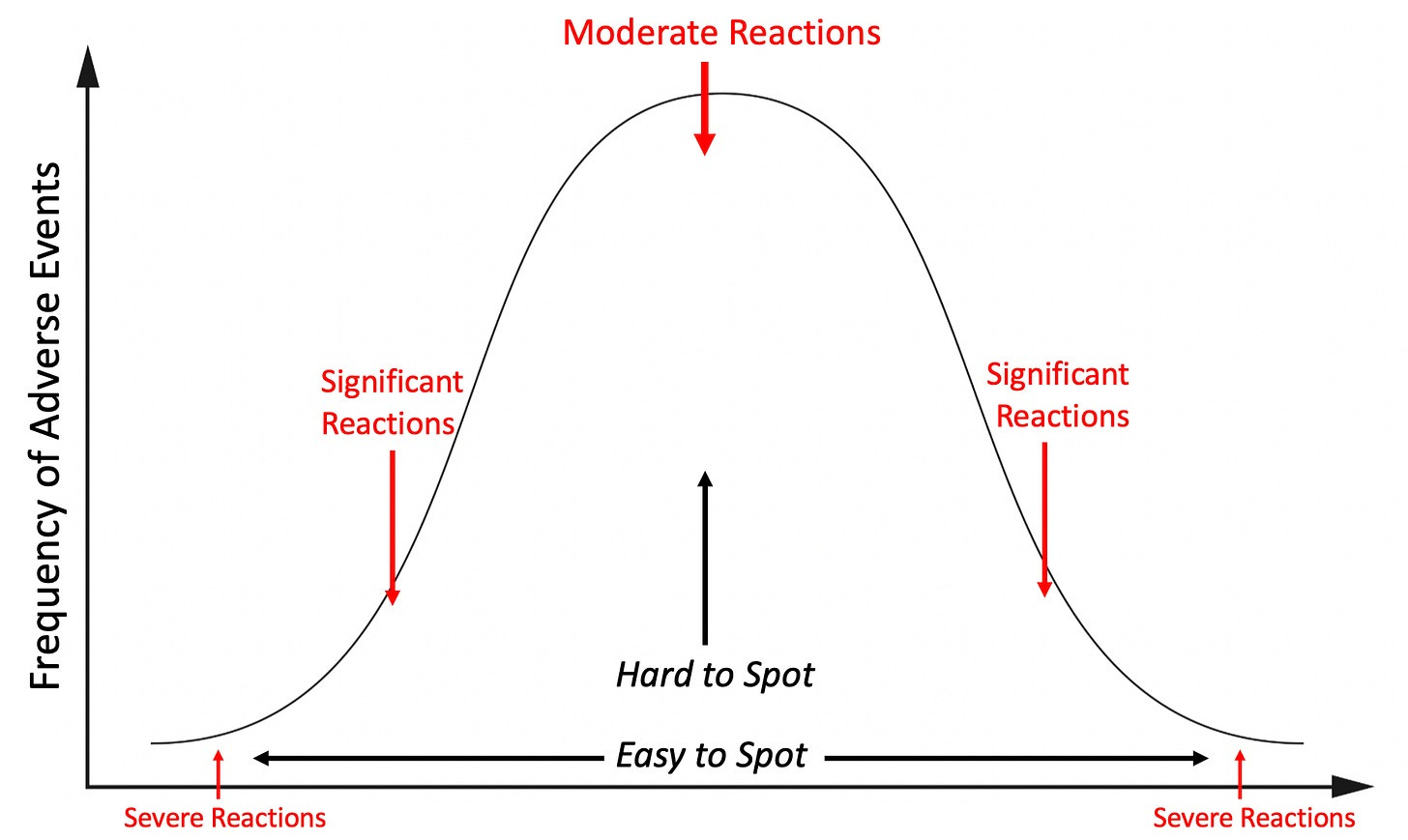
But here’s what those complaints actually included—and this is where it gets uncomfortable.
Reports of extreme agitation.
Sudden personality changes.
Suicidal thoughts.
And in some cases, violent or psychotic behavior.
These weren’t isolated incidents. They showed up early, and they showed up often enough to raise serious concern.
However, the narrative that followed was clean and confident.
These drugs are safe.
They correct a serotonin imbalance.
They help restore normal function.
That framing shaped decades of medical thinking—and it still hasn’t been fully revisited.
But when you move past the marketing and look at patient experiences, a very different picture starts to take shape.
Not just rare or extreme reactions, but widespread, everyday changes that affect how people feel, think, and relate to the world around them.
In one survey of 1,829 patients taking antidepressants, the numbers were striking.
→ 62% reported sexual dysfunction.
→ 60% said they felt emotionally numb.
→ 52% felt like they weren’t themselves anymore.
That’s not a rare side effect profile.
That’s the majority experience. For people struggling with their mental health.
I don’t know about you, but something about this just doesn’t sit right.
What makes it even more concerning is that many of those patients said they were never warned of the possible side effects before starting treatment.
Not about the emotional blunting.
Not about the sexual dysfunction.
Not about how these drugs could fundamentally change how they experience life.
And for something this common, that lack of warning is hard to ignore.
So people go in expecting relief from depression…
And instead, some come out feeling disconnected from their emotions, their relationships, and even their own identity.
Not worse in a dramatic way—but altered in a way that’s hard to explain and not something they had on their radar.
What patients actually experience on antidepressants often sounds nothing like what they were promised.
The full breakdown from A Midwestern Doctor shows how common these effects are—and why so many people say they were caught off guard.
The Truth About SSRI Antidepressants
Let’s look at their effectiveness, because this is where things get even more interesting.
Across clinical trials, the difference between antidepressants and placebos is consistently very small.
And it wasn’t just small—it was inconvenient.
In some cases, researchers had to creatively restructure trial data to make the drug appear effective.
There are even documented claims that early approval processes involved serious irregularities, including testimony that key negative outcomes were not properly reported.
That shifts this from a scientific debate… to a credibility problem.
And there’s a detail here that most people never hear:
When researchers gave patients “active” placebos—ones that produced noticeable side effects—the apparent benefit of antidepressants disappeared.
If the benefit goes away when patients can’t tell whether they’re on the drug or not, then part of what we’re seeing may not be the drug correcting anything biologically.
Read that part again.
Instead, it suggests something more subtle.
The side effects themselves signal to the patient that they’re receiving treatment.
And that belief—the expectation that something is happening—can influence how they feel.
That’s not the same thing as fixing an underlying chemical imbalance.
Full stop.
Now look at behavior.
If a drug is working well, people tend to stay on it. But that’s not what we see with antidepressants.
One study of over 7,500 patients found that 56% stopped taking SSRIs within just four months.
Another survey found 81.5% weren’t even sure the medication was necessary.
That’s a striking level of uncertainty that should give anyone pause before starting an SSRI.
It suggests many people are taking these drugs without feeling clear, consistent benefits.
And many are deciding to walk away from them fairly quickly.
So why are they still being prescribed so much?
The most difficult part of antidepressants isn’t always starting them.
It’s what happens when you try to stop.
And that’s where many people begin to realize something deeper is going on.
A Midwestern Doctor goes into all the details. If you’re planning on taking or are taking an SSRI, you need to read this.
The Truth About SSRI Antidepressants
There are also serious safety concerns that rarely get discussed in everyday conversations.
A Cochrane review found that SSRIs double the risk of suicide.
And in one study of healthy volunteers, 10% became suicidal after taking Zoloft.
That’s shocking. Aren’t some of these people already at risk of suicide? What if, for some people, these medications just making it worse?
There’s another effect that almost never gets discussed.
SSRIs can actually trigger bipolar disorder in some patients.
In one large review, about 7.7% of patients developed bipolar symptoms each year after starting these drugs—roughly triple the expected rate.
In other words, a medication meant to stabilize mood… can push some people into a more unstable condition.
Huh?!
Then there are the real-world experiences that don’t show up neatly in data tables.
A teenager says, “You don’t know what it’s like in my head,” after a sudden shift in mental state.
Another person describes sitting on the floor, overwhelmed, convinced they’re losing their mind.
And for some, the effects don’t fully reverse even if they stop taking them.
One patient shared a shocking description: “I feel like my soul was ripped out of my body.”
This isn’t just about mood changes.
It’s about how people experience reality itself—how they connect, feel, relate, and find meaning in everyday life.
And when that shifts, it’s not always easy to get it back.
Doctors even have a name for one of the most common effects: emotional blunting.
Studies suggest it affects somewhere between 40% and 60% of users.
That means a large portion of people aren’t just feeling less depressed—they’re feeling less of everything.
Is that worth it? Is that really a solution?
One of the most controversial areas is pregnancy.
SSRIs are still commonly prescribed to pregnant women, despite evidence showing increased risks.
Studies have linked them to higher rates of premature birth, heart defects, and even a several-fold increase in a serious condition called pulmonary hypertension in newborns.
These aren’t minor side effects. They affect an entirely different life.
And then comes withdrawal, which may be the least understood part of the entire situation.
A meta-analysis found that 56% of patients experience withdrawal symptoms when stopping SSRIs, and 46% of those cases are severe.
People describe brain zaps, dizziness, panic surges, insomnia, intense mood swings, and a sense that something is deeply wrong.
And when they go back for help, they’re often told those symptoms mean they need the medication.
This can obviously create a difficult loop to break.
The drug changes how the brain functions. Stopping it creates distress. That distress is interpreted as illness. The drug is continued or increased to treat the “illness.”
Over time, that loop can lead to multiple medications being layered on top of each other.
Not necessarily to treat the original issue—but to manage the effects created along the way.
That doesn’t seem like a healthy loop to get trapped in.
This isn’t about saying antidepressants never help.
Some people do benefit from them, and that matters.
But it’s also worth acknowledging something that’s quietly shifted in recent years.
The idea that depression is caused by a simple “chemical imbalance” in the brain was never conclusively proven—and even parts of the medical community have started stepping away from that explanation.
The scale of use—and the gap between expectation and reality—absolutely deserves a closer look.
Because when you step back and look at the full picture—the limited advantage over placebo, the widespread emotional blunting, the dropout rates, and the difficulty of coming off these drugs—it stops looking like a simple treatment story.
It starts looking like something that expanded faster than the evidence supporting it.
And that raises a simple, uncomfortable question:
Are we fully understanding what these drugs are actually doing?
Thanks for reading! This information was based on a report originally published by A Midwestern Doctor. Key details were streamlined and editorialized for clarity and impact. Read the original report here.
The Truth About SSRI Antidepressants
For a deeper dive into what modern medicine has overlooked—or intentionally buried—check out these other eye-opening reports by A Midwestern Doctor:
The Great Alzheimer’s Scam and The Proven Cures They’ve Buried for Billions
The FDA’s 50-Year War on the Safest Painkiller Ever Discovered
What’s The Healthiest Water To Drink?
While you’re at it, give A Midwestern Doctor a follow. No one brings more research, clinical insight, or historical context when it comes to exposing the health myths we’ve all been fed. This is easily one of the most valuable accounts you’ll ever follow.
If you haven’t subscribed to this Substack yet, take a moment to read what some of the most powerful voices in the medical freedom/truth movement have to say:
“The Vigilant Fox has been putting in a lot of work to create a news platform that shares the stories we want to hear about and brings attention to the most important things to know about. If you want a daily newsfeed in alignment with our ...”
– A Midwestern Doctor, The Forgotten Side of Medicine
“The Vigilant Fox absolutely is on top of things. We must support our fighters, and the Fox is fighting with truth.”
– Tom Renz, Tom Renz’s Newsletter
“Excellent capture of key video presentations on evolving pandemic science.”
– Peter A. McCullough, MD, MPH, FOCAL POINTS (Courageous Discourse)


























I had a foray into hell as a result of 3 months of Paxil, lost a 6 figure a year job, bought a corvette and got a crazy meth head for a girlfriend. My marriage almost ended and I had numerous close calls with high speed and dangerous people. Coming off it was like continuously being electrocuted, this lasted for a couple of years. The only way to mitigate the side effects was heavy consumption of moose drool and Guinness and the strongest cannabis I could find. This seemed to take the edge off but made life a bit more challenging. Nancy was right drugs are bad, just say no, unless it grows or occurs naturally then you need to take as much as humanly possible. After years of cannabis consumption and dark beer I finally emerged into a somewhat comfortable spot but it took a decade and cost me hundreds of thousands. We are owed everything by these pharmaceutical companies, no amount of compensation would come close to the damage on our society, add opioids, gabapentin, adhd drugs and were are talking about almost the entire adult population. We were all completely fucked over so they could make a buck. Capitalism at its finest. Ask me again why I don’t trust any American doctors, I wouldn’t let them trim my toenails as they would just cut your toes off so you don’t have that problem.
I had two antidepressant induced suicide attempts. These drugs are over used and dangerous. Cchr.com